The year is 2042. Mr. Suresh is not feeling well. He is breathless and there is a pain in the chest when he tries to walk. It had been there for some time. But now, he had to see a Doctor.he doctor finds out that his heart is failing. It is sort of irreparable.
Suresh is not scared. The doctor doesn’t scare him by his words either.
A little bit of blood is taken from Suresh. And he is asked to come back after two weeks. Some medicines are given for the symptoms.
Meanwhile, the lab gets busy. From his blood, cells called stem cells are isolated. From these cells, by a complex series of steps, the following cells are grown in test tubes: heart muscle cells, cells to line the heart chambers and coronary vessels, and cells that make up the conducting system of the heart.
A net like model of the heart is made – called a scaffold, using complex biomaterials. Or the scaffold could be made from a pig’s heart, by leaching out all the cells, and keeping only the fibrous, non-cellular ghost of the heart.
Then, the cells are systematically seeded into the scaffold and allowed to grow.
Suresh comes back. He is taken in for a small operation:
Take out the old heart. Put in the new heart. That is all. Suresh goes home smiling.
Similarly, livers, kidneys, pancreas, and even hands and legs can be similarly made in the lab, with the patient’s own cells.
During my childhood, my father had a car. When it needs repair, it was all tinkering. Hammer, bend, oil, and very occasionally, change a fuse or rubber valve.
Now it is always replacement. A module is damaged? Take it out and put a new one in. The extreme reliability of my car contrasts with the frequent breakdowns of my father’s.
A year back, I had written an article in Deccan Chronicle about research that tries to turn spinach leaves into a system of finely branching tubes lined by cellulose that can mimic the arborizing network of blood vessels which supply most organs. The article came out in the journal Biomaterials.
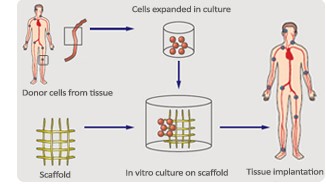
These are part of an ongoing attempt to generate tissues and even organs that can be used to replace diseased human ones.
Comparing a car to sentient Human beings may offend some people. But essentially, we are incredibly complex machines, designed by millions of years of evolution. Our thinking, scheming, philosophizing, loving, empathizing, exulting, and personality-generating human brain is supported by intricate pumps, filters, factories and mobile moving parts.
Many of our diseases involve abnormalities in key organs like the heart, liver and kidney. Cancers and accidents may take away parts of the body, like hands, legs and breasts. Crucial parts like jaws, noses and others can go when we do cancer surgery.
Tinkering has its limits. We can continue to treat heart disease, but ultimately, a severely diseased heart will fail, and the person will die. Similar is true for liver, intestines and kidney.
Plastic and Reconstructive Microsurgery has come a long way. Now we can take the fibula, one of the bones in the leg that is not needed for walking, along with its blood supply, and replace a jaw bone by shaping it and connecting to blood vessels in the neck. Skin, muscles etc can be transferred from one part of the body to another.
But it is surely not the same as taking a smear of cells from one’s mouth or a few from the blood, growing them in the lab after turning them into bone cells and seeding them into special frameworks shaped exactly like a jawbone and then implanting them onto the face.
Imagine – if a patient is suffering from heart failure, we can take a 3D printed scaffold, shaped just like his heart, modelled on a CT Scan of it, seed his own cells after converting the stem cells from his blood into cardiac muscle cells, and make a heart. This is what Tissue Engineering is all about.
The main challenge has been to find ways of supplying blood to tissue-engineered organs and body parts. This where research like what has been described with a spinach leaf comes in. A network of fine, bio-compatible tubes is what we want.
Till now, our only method of true replacement-medicine has been transplantation of organs from another person. It can be either from a live donor when an extra organ is available (like kidney), or from brain-dead bodies, unfortunately in that state by accidents or disease. The supply of organs is obviously severely limited. And patients require lifelong, costly, sometimes crippling and occasionally dangerous immune suppressing medicines to prevent rejection of another person’s organ from the body.
We can grow stem cells now from adult cells. Previously we could get them only from embryonic cells. Intense research is going on in this area right now. Lab work on embryonic stem cells is strictly regulated by law. We can grow sheets of cartilage, bone, or skin cells in the test tube. Sheets of epidermal skin cells are already in use for treatment of burns.
Scaffolds are being perfected. An ear scaffold has been seeded with cartilage cells and was grown on the back of a mouse as an experimental project. Bone cells were seeded into scaffolds shaped like some facial bones and then they were implanted into muscles. These shaped bones were transferred by taking the blood vessels of the muscles, along with the attached artificial bone and muscle, and then doing microsurgery to put it in patients who had to have their facial bones removed for cancer. It is not routine, but it has been done.

Ear On A Mouse!
Sometime in the future we will surely reach that stage when custom made organs and body parts are possible. That will be a true revolution in Medicine. Have no doubt – that is the next BIG thing.
Who knows- a time may come when any organ, or body part- heart, intestine, and even entire complex part of the body like the chest cavity with all its organs, or the entire abdomen, can be grown from a single stem cell of our body. After all, we are all grown from a single cell derived from the fusion of our father’s sperm and the mother’s egg.
It may not take a hundred years. After all, objects in the mirror are closer than they appear.



Valuable article….